Transcatheter aortic valve implantation (TAVI) is an established alternative to surgical valve replacement in the management of calcified severe aortic stenosis in those with co-morbidities or adverse features (advanced age, impaired left ventricular function), or in those where open surgery may be associated with unfavourable technical features, such as previous sternotomy with a patent internal mammary graft, porcelain aorta or previous thoracic radiation, rendering the operative field hostile.1–3 A large body of experience and evidence exists predominantly for two commonly used TAVI devices; namely the balloon-expandable Edwards Sapien Valve (ESV) (Edwards Lifesciences Ltd, Irvine, California, US) and the self-expanding Medtronic CoreValve (MCV) (Medtronic Inc, Minneapolis, Minnesota, US). Although the fundamental principle behind the two valves is similar, both involving a stent with three bioprosthetic cusps (leaflets) deployed within a calcified native aortic valve, the specific design features and potential indications are different. In this article we explore in detail the respective design features, related indications for each valve type as well as their known outcomes.
General Indications for Aortic Valve Implantation
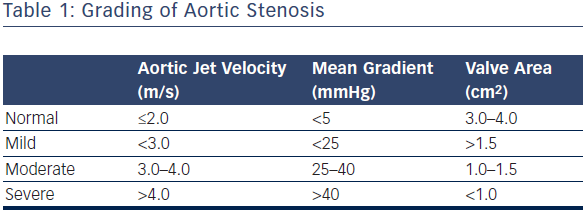
Normal aortic valve area is between 3 and 4 cm2 and a transvalvular gradient develops when the valve area decreases by half. Patients with a normal left ventricle are generally asymptomatic unless the valve area is <1 cm2, with an accompanying jet velocity of approximately 4 m/s and a mean gradient >40 mmHg (see Table 1).4 Symptoms may occur at lower gradients and with less obstruction in some patients, such as those with poor left ventricular function (low flow aortic stenosis).
Besides native aortic valve disease, it is important to consider that surgically implanted bioprosthetic valves also undergo structural deterioration resulting in calcification, wear and tear, thrombosis, pannus formation and docarditis.5 This deterioration can manifest as aortic stenosis, regurgitation or mixed disease. Although in a bid to avoid redo surgery, valve-in-valve TAVI is emerging as a treatment option in this group of patients, it is beyond the scope of this article.1
Patient Selection Criteria and Contraindications for Transcatheter Aortic Valve Implantation
The patient selection criteria for TAVI are essentially the same as for surgical valve replacement. The main reason for opting for TAVI is the presence of co-morbidities placing the patient in either the inoperable or the high-risk category, making the option of open surgery less favourable. Current recommended patient selection criteria for TAVI from the European Association of Cardio-Thoracic Surgery (EACTS) include one or more of the following:6
- European System for Cardiac Operative Risk Evaluation (EuroSCORE) >20.
- Society of Thoracic Surgeons (STS) score >10.
- Presence of factors not covered in risk scores, such as challenging surgical cases (porcelain aorta, previous thoracic radiation, coronary artery surgery with a patent mammary artery graft) and the presence of severe co-morbidities.
Numerous exclusion criteria are present, although none are absolute. The presence of a bicuspid, unicuspid or non-calcified aortic valve, severe aortic regurgitation (AR) and a native annulus size that is too small or too big relative to available TAVI devices (currently unsuitable annulus sizes include <18 mm or >29 mm for a MCV prosthesis
and <18 mm or >27 mm for an ESV prosthesis) are some excluding factors.7–9 In addition, expected patient survival of less than one year, a dilated ascending aorta at the sinotubular junction (>45 mm for the MCV prosthesis) and the presence of apical thrombus are also considered to be contraindications.6
Differences in Transcatheter Heart Valve Design
Edwards Sapien and Sapien XT Valve
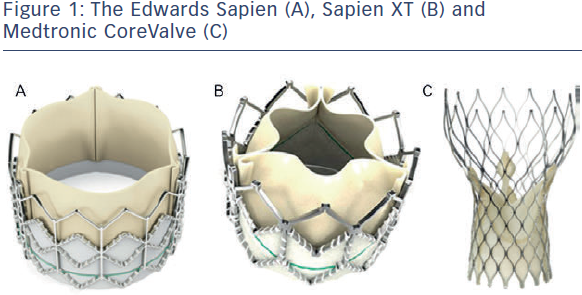
The Edwards Sapien valve (ESV) (see Figure 1A) has been in use since 2006. It consists of a balloon-expandable stainless steel frame and three bovine pericardium cusps (leaflets) mounted onto a polyethylene terephthalate skirt (PET). Transfemoral delivery is facilitated via the RetroFlex 3 system, and the Ascendra system is used for transapical implantation. The newer generation Sapien XT valve, introduced in 2010 (see Figure 1B) consists of a balloon-expandable cobalt chromium frame with bovine pericardium cusps (leaflets). For transfemoral implantation the valve is crimped onto the NovaFlex delivery catheter and introduced via a sheath into the femoral artery. Transapical and transaortic delivery are also possible using the Ascendra 2 or Ascendra plus systems. Rapid pacing is required during deployment as the valve is balloon expandable. Both valves are available in 23 mm and 26 mm sizes, although more recently, the Sapien XT has been introduced in a 29 mm size, enabling treatment of annular diameters between 18 and 27 mm. The newer generation Sapien 3 valve underwent first-in-human implantation in 2012. In comparison with the Sapien and Sapien XT valve this has a lower crimp profile and an additional outer PET skirt to reduce paravalvular regurgitation. This valve is not discussed further in this article.
Medtronic CoreValve
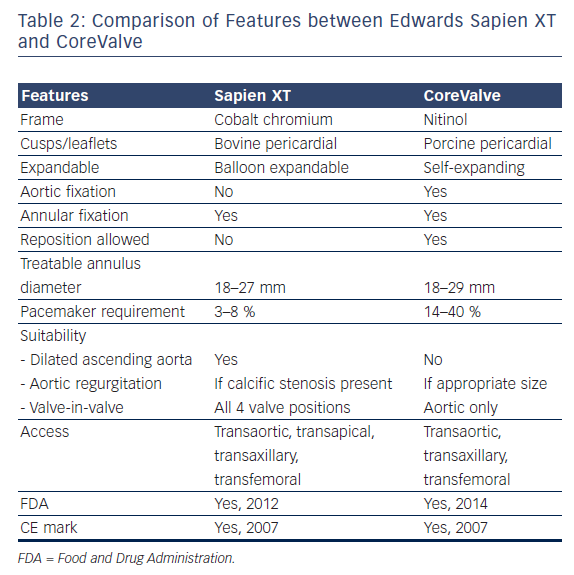
The Medtronic CoreValve (MCV) consists of a nitinol self-expandable frame and porcine pericardial cusps (leaflets) mounted onto a porcine pericardium skirt (see Figure 1C). Nitinol, an alloy of nickel and titanium, exhibits martensitic transformation, which allows it to undergo a fully reversible solid-state transformation. Accordingly, at higher temperatures (e.g. body temperature) nickel exists as austenite, a strong cubic structure, whereas at lower temperatures (e.g. in an ice bath) it exists as martensite, a monoclinic crystal structure, exhibiting superelasticity, making it 10–30 times more elastic than other metals. This property allows it to be tightly compressed into a delivery sheath for implantation via the transarterial route (aortic or femoral).10 Currently, sizes 26, 29 and 31 mm are available. The next generation CoreValve Evolut valve is now available in 23 mm, and once in routine use, the range of treatable annular diameters will be between 17 and 29 mm. Table 2 details the differences between the ESV and MCV.
Indications for Each Valve Type
There are several factors to consider when contemplating a valve type and method of delivery. These include:
- native annulus size;
- cardiac anatomy;
- peripheral arterial assessment; and
- risk of annular rupture.
Native Annulus Size
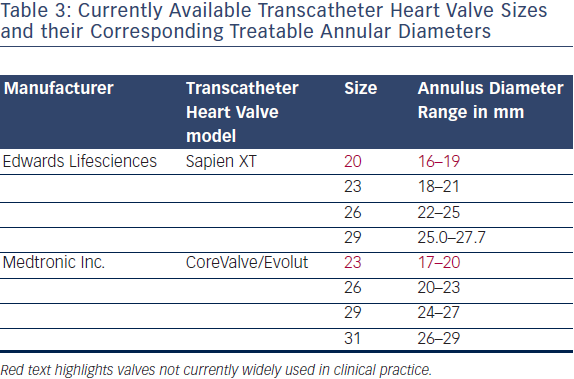
Accurate assessment of the native annulus should be at the forefront when considering a TAVI procedure. It is a given that an annulus size of <18 mm or >29 mm precludes any form of TAVI at present. Since there is no current imaging gold standards for annular assessment, a combination of several methods may be employed, including transthoracic and transoesophageal echocardiography in addition to computed tomography (CT) and magnetic resonance imaging (MRI).3 Available valve sizes and their appropriate corresponding native annulus sizes are given in Table 3. It is worth mentioning that at present, until smaller sizes of MCV (Evolut 23 mm) and ESV Sapien XT (20 mm) become available for routine clinical use, a size 23 mm ESV is suitable for a native annulus size of 18–20 mm and MCV 31 for 27–29 mm annular diameters.9 Finally a degree of relative oversize (5–10 %) is required with the ESV system to minimise the risk of paravalvular regurgitation.1
Cardiac Anatomy
In addition to annular diameter, a detailed assessment of cardiac anatomy is necessary as this can affect the choice of implant and method of delivery. Specifically, it is important to acknowledge specific structural variations:3
- Bicuspid aortic valve – the elliptical shape of the valve orifice in this condition is considered a relative contraindication to TAVI as it may result in higher rates of paravalvular regurgitation when implanting a cylindrical prosthesis. In more experienced hands, however, a slightly higher than normally positioned MCV may provide a good result.11,12
- Left ventricular outflow size and shape is another consideration. The presence of a sigmoid-shaped septum or an existing mitral prosthesis may make transapical delivery more suited and hence favour the ESV.
- A porcelain aorta and a horizontally placed aortic root may make transfemoral delivery more challenging and risky thereby favouring a transapical or transaortic delivery of an ESV. However, with experience and improved delivery systems, transfemoral placement is becoming more feasible and predictable.
- The presence of a mitral valve prosthesis requires special consideration. Too low a placement of the transcatheter heart valve (THV) must be avoided as this can cause interference with mitral valve function.
- The height of the coronary artery ostia should be at least 10 mm from the base of the aortic valve to prevent occlusion of the coronaries following THV implantation.
- Although there is always some degree of valvular calcification, the presence of a large calcific nodule can cause coronary occlusion on THV implantation.
Peripheral Arterial Assessment
Accurate assessment of the peripheral arterial tree is crucial when considering an ideal method of delivery and the type of implant.3 Current methods of assessment include CT and peripheral angiography. In general, an ilio-femoral diameter <6 mm is considered unsuitable for transfemoral TAVI. The presence of ilio-femoral tortuosities, kinks in the aorta, existing stents, aneurysms or thrombi are also contraindications for transfemoral access, and alternative access via the transapical, transaortic or subclavian route have to be considered.
Risk of Annular Rupture
Aggressive balloon dilatation and oversizing during TAVI using the ESV has been associated with aortic root and annulus rupture.13 In a study of 37 consecutive patients with left ventricular outflow tract (LVOT) rupture during ESV deployment, a higher degree of sub-annular LVOT calcification (Agatston score), higher frequency of oversizing (by >20 %) as well as balloon post-dilatation were all associated with a higher risk of annular rupture.14 It is possible that the introduction of the Sapien 3 valve may reduce the risk of annular rupture as relatively less oversizing is required.
Differences in Outcomes
In addition to self-reported registry data, randomised data are available from the Placement of Aortic Transcatheter Valves (PARTNER) trial, which evaluated the ESV, and the CoreValve US Pivotal trial, which evaluated the MCV. The retrospective Pooled Rotterdam - Milano Collaboration (PRAGMATIC) study compared the two valves and the recent Comparison of Transcatheter Heart Valves in High Risk Patients With Severe Aortic Stenosis (CHOICE) study is the only randomised control trial of the two devices. In summary, although device specific complications are evident, there are no differences in clinical outcomes in terms of short- or long-term survival with use of either valve.15 Details of registry data and the relevant trials are presented below.
Edwards Sapien Valve
PARTNER TRIAL
The PARTNER trial consisted of two parallel arms. In cohort A, standard surgical aortic valve replacement (SAVR) was compared with TAVI in high-risk patients as determined by a STS score of >10 % and/or predicted operative mortality of 15 % or more. In cohort B, TAVI was compared with medical management (including balloon valvuloplasty) in inoperable patients with severe aortic stenosis. Patients enrolled into this cohort were deemed to have an operable risk of >50 %.
The one-year results from the trial demonstrated that in cohort A, TAVI and SAVR were found to be equivalent in terms of overall mortality, with all-cause mortality from TAVI at 24.2 % and 26.8 % from SAVR. Although the rate of stroke following TAVI was higher at 5.1 % compared with 2.4 % following SAVR, this result did not reach statistical significance. Results from cohort B confirmed that TAVI was superior to medical management, with the mortality rate from TAVI at 30.7 % compared with 50.7 % from medical treatment. There was, however, a higher rate of major vascular complications and stroke in the TAVI group compared with the conservatively managed group.
Review of the two-year data showed that the rate of stroke was 11.2 % with TAVI and 6.5 % with SAVR (p=0.05), and mortality in cohort A was 33.9 % from TAVI compared with 35.0 % from SAVR. Additionally, although paravalvular regurgitation was noted to be moderate in 7.0 % and severe in 1.9 % at one-year, this had decreased to 6.9 % and 0.9 %, respectively at two years, (p<0.001 for both intervals). Nonetheless, even mild paravalvular regurgitation was associated with an increased mortality (p<0.001).
Important findings from cohort B showed that mortality from TAVI was 43.3 % in the TAVI group compared with 68.0 % in the medical group, (p<0.05).15–17
SOURCE Registry
The Edwards SAPIEN Aortic Bioprosthesis European Outcome (SOURCE) Registry is the largest series of consecutively ESV implanted TAVI patients with one-year outcomes. A total of 2,344 consecutive patients were enrolled in two cohorts to reflect trends overtime. Cohort 1 consisted of 1,038 patients enrolled at 32 European centres between November 2007 and January 2009. Transfemoral TAVI was undertaken in 463 patients and transapical in 575 patients. The overall one-year survival was 76.1 %; 72.1 % for transapical and 81.1 % for transfemoral access. The transapical group represented a higher-risk population, given that the logistic EuroSCORE for this group was significantly higher than that of the transfemoral TAVI patients.
Cohort 2 of the Registry consisted of a further 1,306 consecutive patients at 37 European centres enrolled between February 2009 and December 2009. Final results from the SOURCE registry indicated excellent results, with two-year survival at 67.7 % overall, similar stroke risks between the two cohorts of 2.5 % in cohort 1 and 2.8 % in cohort 2, which notably were lower than the 30 day stroke risk from transapical TAVI in cohort A of the PARTNER trial at 3.8 %.18,19
Medtronic CoreValve
ADVANCE Study
The MCV ADVANCE Study is the largest multicentre prospective MCV study comprising of 1,015 patients treated at 44 centres in 12 countries. The stroke rate in this group of patients was lower than the PARTNER A cohort at 4.5 %, and the one-year all-cause mortality rate was better than PARTNER A; 17.9 % compared with 24.2 %. These results were an improvement on previous pre-dated registry data such as FRANCE-2 and the UK registry (see below).20
CoreValve US Pivotal Trial
This prospective, randomised controlled multicentre trial of 795 patients in 45 centres in the US compared the MCV with SAVR in high-risk patients. The primary endpoint was the risk of death from any cause at one-year.
All-cause mortality at one-year was 14.2 % in the MCV group versus 19.1 % in the SAVR group. In addition, lower rates of cardiovascular and cerebrovascular events were noted in the TAVI group. In contrast to PARTNER A, this study did not show a higher rate of stroke post-TAVI when compared with rates post-SAVR.
The incidence of moderate to severe AR post-TAVI at one-year was 6.1 %, although this did not have an adverse effect on survival. In the majority of patients (76.2 %) discharged with moderate to severe AR, this had reduced to mild or none on one-year follow-up. Possible explanations given were the properties of nitinol, a higher placement and more accurate pre-TAVI assessment of the annulus with CT.21
Weighted Meta-analysis of Early and Late Clinical Outcomes after CoreValve Transcatheter Aortic Valve Implantation in Seven National Registries
This meta-analysis included 2,156 patients treated with the MCV prosthesis between 2007 and 2010 in seven countries. Reported results included early (30-day) outcomes including procedural success, stroke and pacemaker rates as well as one-year survival rates. Pooled procedural success was 97.8 %, the stroke rate was 2.8 % and the pacemaker implantation rate was 28.7 %. Early survival was 93.4 % and one-year mortality was 17.1 %. Limitations of this meta-analysis by virtue of its design included the variability in patient selection criteria, the non-standardised definitions of adverse events and the under reporting of clinical events.22
CoreValve Versus Sapien Valve
CHOICE Randomised Clinical Trial
The CHOICE study is the only randomised controlled trial (RCT) comparing a self-expandable valve (MCV) to a balloon-expandable valve (ESV). In this trial the primary endpoint was device success as measured by: successful vascular access; and deployment and retrieval without the need for a second valve; and less than mild AR post-procedure. Secondary endpoints included the need for a permanent pacemaker system, cardiovascular and all-cause mortality at 30 days.
Results from this trial showed that although cardiovascular mortality, bleeding and vascular complications were similar for both valves, there was a higher risk of pacemaker insertion following MCV implantation, a lower rate of more than mild AR following ESV implantation and better device success with the ESV valve (95.5 % versus 77.5 % p<0.001).23
PRAGMATIC Study
The aim of the PRAGMATIC study was to compare outcomes from transfemoral TAVI between the Medtronic CoreValve and Edwards Sapien/XT valves for patients with severe aortic stenosis. This non-randomised, retrospective study analysed pooled data from four experienced European centres, which underwent propensity score matching in view of differences in baseline characteristics. Of a total of 793 possible patients, 204 in each group were identified. There was no difference in 30-day all-cause mortality (MCV 8.8 % versus ESV 6.4 %, p=0.3520), major vascular complications (MCV 9.3 % versus ESV 12.3 %, p=0.340), or one-year all-cause or cardiovascular mortality between the two valves. There was a higher incidence of permanent pacemakers in the MCV group at 22.5 % versus 5.0 % in the ESV group (p≤0.001), which is likely a result of valve design. In addition, this study found that although there was no difference observed in the incidence of AR of any grade between the two valves types, residual moderate to severe AR was associated with an increased one-year mortality.24
UK Registry
Data from the UK TAVI registry evaluated outcomes according to valve type and method of delivery. In essence, there was no significant difference in mortality between the ESV and MCV groups at any timepoints, and no difference in mortality between the two valves types for transfemoral delivery. There was a higher incidence of permanent pacemaker implantation as well as paravalvular regurgitation with the MCV prosthesis. Transapical delivery of the ESV valve was associated with higher mortality at 30 days as well as one-year when compared with transfemoral delivery of the same valve type. Trans-subclavian delivery of the MCV was associated with higher mortality, although this did not reach statistical significance. Cumulative survival for transapically implanted ESV was found to be associated with a lower survival than with transfemoral delivery. Survival rates for subclavian delivery of the MCV cohort initially tracked that of both valves when delivered via the transfemoral route, but at six months this fell dramatically, meeting the poorer survival rates for transapically delivered ESV.2
FRANCE 2 Registry
This study was a prospective multicentre study of the French national TAVI registry. The primary endpoint was death from any cause. A total of 3,195 patients were included, having undergone TAVI using the ESV and the MCV between January 2010 and October 2011, at 34 centres. Results from this study were comparable with the PARTNER trial in terms of mortality at 30 days (9.7 %) and one-year (24 %). MCV use as associated with a higher rate of permanent pacemaker (PPM) as well as periprosthetic regurgitation. Multivariate analysis indicated that a higher logistic EuroSCORE and transapical approach as well as residual paravalvular regurgitation was associated with an increased mortality.25
Meta-analysis of Impact, Incidence and Predictors of Aortic Regurgitation after Transcatheter Aortic Valve Implantation
This meta-analysis of 45 studies included a total of 12,926 patients. Results indicated that AR was common post-TAVI and was an adverse prognostic indicator of short and long-term survival. AR was also more prevalent in the MCV group at 16.1 % versus 9.1 % in the ESV group (p=0.005).26
Conclusions
TAVI is a suitable alternative to surgical valve replacement in inoperable and a select group of high-risk patients with severe symptomatic aortic stenosis. Significant technological and device design advances have occurred since the first TAVI was performed. Two devices in current use are the MCV and the ESV. Although device design features may vary and individual device complications may be present, studies have not shown a difference in mortality between the two valve types. At present, device choice is dictated by physician preference, annular diameter and, in a small percentage of patients, by availability of transapical access route for ESV. It is unclear at present which of the two devices is better with respect to degree of AR, as it may be dictated by local anatomy rather than device choice; although due to its specific design features, the MCV was found in some studies to be associated with a higher rate of AR, which did decline overtime, perhaps explaining the lack of difference in outcome data between the two valves. The MCV was also found to be associated with a higher rate of permanent pacemaker implantation, and along with AR, these factors may well become more important if TAVI is introduced into a lower risk population.